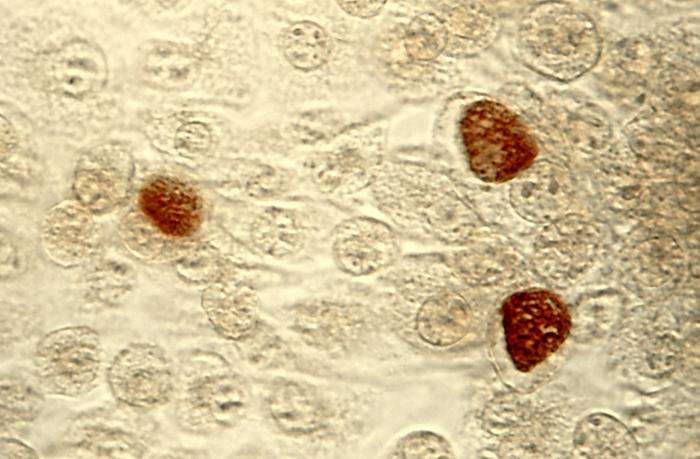
Anyone sexually active under age 30 should be offered testing for chlamydia and gonorrhea, according to a new guideline from the Canadian Task Force on Preventive Health Care published in CMAJ (Canadian Medical Association Journal).
Chlamydia and gonorrhea are the most commonly reported sexually transmitted bacterial infections (STIs) in Canada and are treatable with antibiotics. Without treatment, these infections can lead to pelvic inflammatory disease, pain and possibly infertility.
“If people are under 30 and sexually active, it’s a good idea to get tested,” says Dr. Ainsley Moore, a family physician and associate clinical professor, Department of Family Medicine, McMaster University, and chair of the task force chlamydia and gonorrhea working group. “Many people are asymptomatic and may not seek treatment so we’re recommending opportunistic testing—that is, at any health care visit.”
The guideline recommends that health care providers in Canada offer routine testing for chlamydia and gonorrhea annually to all sexually active patients younger than 30 who are not known to belong to a high-risk group. Sexual activity is defined as anyone who has had oral, vaginal or anal intercourse.
Why is the task force recommending screening?
- 1 in 20 sexually active individuals 15-29 years old will get chlamydia.
- Reported rates for this age group are 1.0%-1.9% (chlamydia) and 0.2%-0.3% (gonorrhea).
- Many people are asymptomatic or do not seek care and are not included in reported cases.
- True rates of chlamydia in 15- to 29-year-olds may be as high as 5%-7%.
- Rising rates of chlamydia and gonorrhea in people aged 25-29 years since 2000.
- Screening may reduce pelvic inflammatory disease in females.
This recommendation does not apply to pregnant people, people known to the clinician to be at increased risk based on sexual behaviours, or patients seeking care for a possible STI. Clinicians should consult national, provincial, or local guidance when providing care for these individuals.
Current practice in Canada recommends screening sexually active people who are not at high risk up to age 25.
“This recommendation to extend screening to age 30 reflects increasing rates of infection among Canadians aged 25 to 29 years,” says Dr. Donna Reynolds, a member of the working group, family physician and an assistant professor at the University of Toronto. “As it’s an easy test, usually a urine test or vaginal swab, it can be done at any visit to a physician, nurse practitioner or sexual health clinic.”
The recommendations also consider the potential for anxiety and embarrassment around screening for STIs.
“Although we recommend this as routine, clinicians know to expect feelings of fear, anxiety or embarrassment on the part of some patients and be ready to discuss these,” says task force member Dr. Brenda Wilson, a public health physician and professor at Memorial University, St. John’s, Newfoundland.
The guideline recommends also screening males as the primary source of infection for females, for whom the health consequences can be greater.
“Screening males, who are often without symptoms, may reduce transmission and complications in females and may improve health equity for females,” says Dr. Moore.
Target Audiences
- Clinicians—The guideline is aimed at clinicians in primary care, sexual health and student clinics and other settings.
- Public—As the guideline is aimed at people younger than 30, an infographic, Instagram campaign and frequently asked questions will help explain why it’s a good idea to get tested.
The task force engaged Canadians to understand their values and preferences around screening to inform recommendations. They expressed a strong preference for screening.
The College of Family Physicians of Canada, the Nurse Practitioner Association of Canada and the Canadian Association of Perinatal and Women’s Health Nurses have endorsed the guideline.
In a related commentary, Drs. Troy Grennan, BC Centre for Disease Control, Vancouver, British Columbia, and Darrell Tan, University of Toronto, write a “potential benefit of the authors” recommendations is its potential to normalize conversations about sexual health and STIs between clinicians and patients, which have long been marred by stigma and shame. Offering screening may help patients feel that they ‘have permission’ to discuss health issues that may seem difficult to talk about.”
Source: Read Full Article
